
From the onset of the COVID-19 pandemic, it was clear that some people adopted recommended safety protocols to help them avoid infection more readily than others.
To better understand the psychological factors underlying this commitment to individual prevention measures, a team of psychology researchers led by Michael Cunningham at the University of Louisville surveyed several groups of people about their attitudes and responses. The studies, published in Frontiers in Psychology in April, revealed associations between individuals’ response to prevention measures and their belief in the credibility of science, control and coping mechanisms and political orientation.
Cunningham and colleagues at UofL, York College in Pennsylvania and FifthTheory, a digital assessment and survey solutions company in Chicago, conducted a series of three online surveys to delve deeper into the psychological determinants of COVID-19 prevention behaviors.
The first study of the series surveyed students, faculty and staff at two higher education institutions in the U.S. The researchers compared respondents’ assessments on the Coronavirus Behavioral Health Mindset (CVBHM), a measure of acceptance of responsibility and adherence to prevention measures, with additional questions to determine respondents’ belief in the credibility of science, political orientation and beliefs about the virus and the degree to which preventing an infection was within an individual’s control.
It showed that those who attributed COVID-19 safety to personal effort rather than inherent ability or outside forces, who had a progressive political orientation and who believed in the credibility of science were more likely to embrace COVID-19 prevention actions such as wearing masks, social distancing and vaccination.
The study began before the COVID-19 vaccine was available, but once the Pfizer vaccine received Emergency Use Authorization from the Food and Drug Administration in December 2020, the team added questions to the survey about willingness to take the vaccine. This gave them insight into attitudes both before and after respondents were confident a vaccine would be a reality.
“The attitudes about the pandemic may differ depending on what you think the solutions are going to be, so issues of sensitization and denial and repression may come in to play slightly differently when you think there is a solution versus when you don’t,” Cunningham said. “We were thinking a vaccine would come but we didn’t all know when it was going to hit, so when it did in December of 2020, that changed the equation quite a bit.”
After the vaccine received authorization, responses to the survey shifted slightly, showing that individuals had become less committed to personal carefulness and health-consciousness to avoid the illness and less likely to believe that becoming ill from the virus was due to fate or luck.
The second study in the series addressed work-related attitudes related to the pandemic. The researchers surveyed adults across the U.S. and found that an intention to be vaccinated corresponded to a willingness to work, less emotional distress and greater focus on customer experience.
The third study documented the personal attributes and motives of individuals who volunteered to help administer vaccines in Kentucky. Nearly 60% of those individuals were motivated by a desire to help others, whereas almost 40% said they volunteered so they could receive the vaccine themselves. Compared to the general population, the survey found the volunteers more likely to be older, to have higher levels of education, to believe in the credibility of science, vote liberal and attribute COVID-19 protection to personal effort.
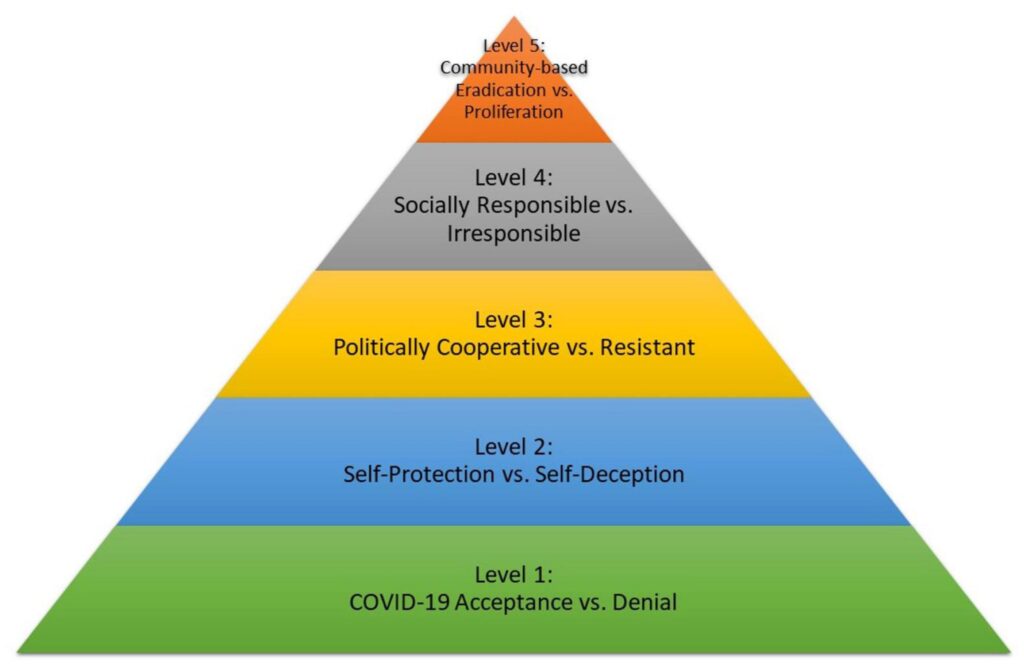
The results of these studies led the researchers to propose a COVID-19 mindset hierarchy model that ranks individuals in terms of their response to pandemic. The model goes from the most basic level 1, acceptance vs. denial of COVID-19, to the most mature level 5, in which individuals become involved in community-based eradication efforts. The knowledge base incorporated in the model is useful in shaping health safety messaging going forward, not only with COVID, but with monkeypox and other plagues that have not yet emerged.
Cunningham and his team are planning additional research to further understand the psychological impact of the pandemic and related losses, to validate the COVID-19 mindset hierarchy and to examine the relation of COVID behaviors to more general health care related topics, such as support for a single-payer system.





























